Pain in the Ball of Your Foot? Understanding Metatarsalgia Symptoms, Causes & Treatment in Mumbai
You've probably felt it — that strange sensation of walking on a small stone, except when you take off your shoe and check, nothing is there. Or the burning ache that builds steadily through the day, starting as a mild discomfort in the morning and becoming sharp and distracting by evening. Sometimes it's a numbness in the second and third toes that comes and goes without obvious explanation.
These are not signs of tired feet. They are the classic early warning signals of metatarsalgia — one of the most common causes of forefoot pain seen at podiatry clinics in Mumbai, and one of the most consistently mismanaged conditions we encounter at Foot Impact.
The reason it gets mismanaged is straightforward. Metatarsalgia is not a diagnosis in itself — it is a symptom of an underlying mechanical problem in the way your foot loads and moves. Treat the symptom without identifying the cause, and the pain keeps coming back. Identify the cause accurately, and most cases resolve fully without surgery, without long recovery periods, and without the cycle of temporary relief followed by relapse that many patients have experienced for months or years before they come to us.
This guide explains exactly what metatarsalgia is, how to recognise it, what causes it, how it is accurately diagnosed, and what treatment at Foot Impact in Mumbai actually involves.
What Is Metatarsalgia — and What Is Actually Happening in Your Foot?
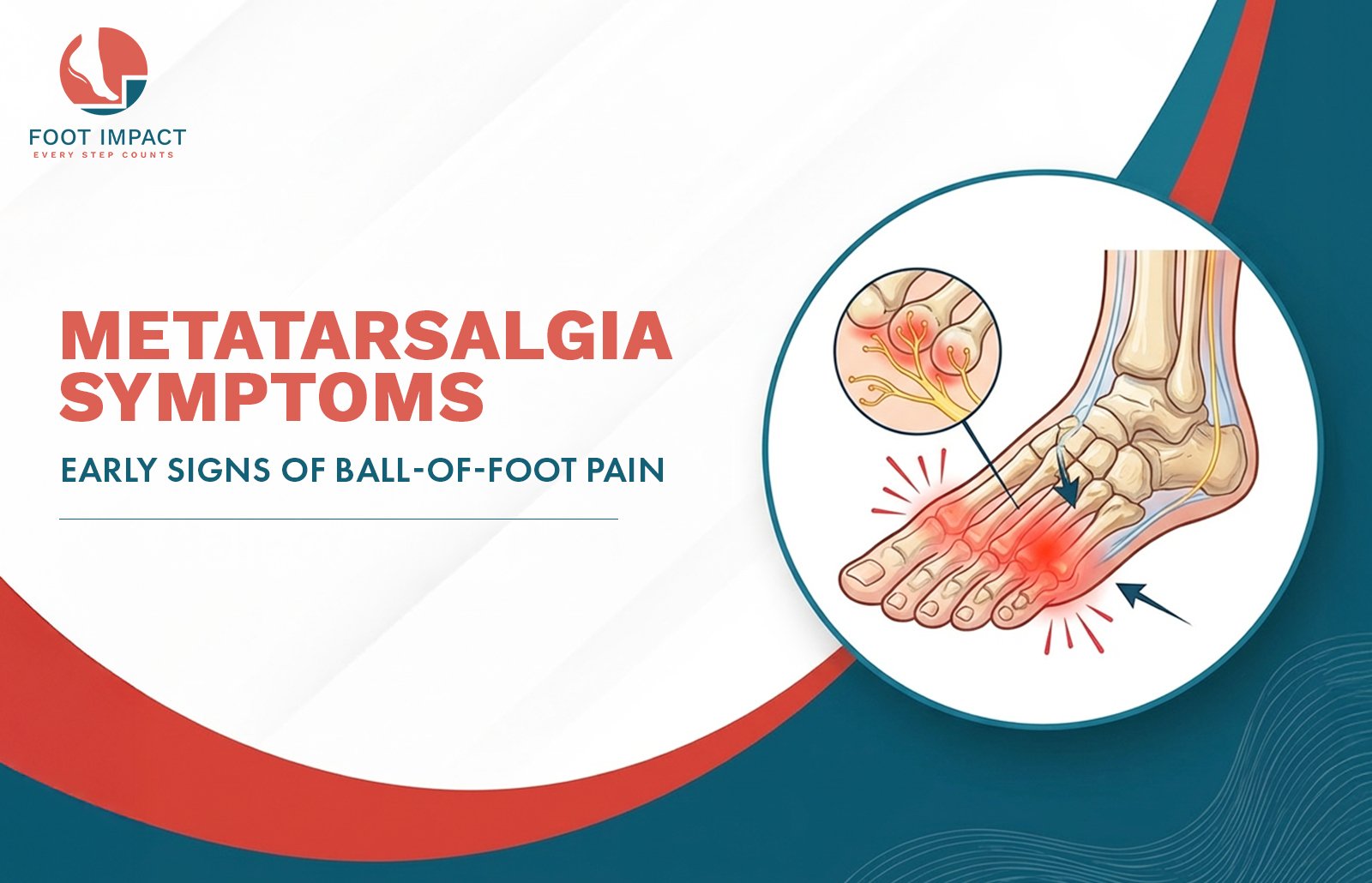
Your foot contains five long bones called metatarsals, running from the midfoot to the base of each toe. At the end of each metatarsal is a rounded head — and it is these metatarsal heads, padded by a thin layer of fat and skin, that bear your body weight every time you push off the ground during walking.
During normal walking, your body weight transfers progressively across all five metatarsal heads in a smooth, even rolling motion. When this load distribution is disrupted — because of foot structure, footwear, weakness in the forefoot muscles, or a change in activity level — one or more metatarsal heads begins absorbing force it was not designed to handle repeatedly. The result is inflammation of the soft tissue, bursa, and nerves surrounding those overloaded metatarsal heads.
This is metatarsalgia. Not a single disease, not a fracture, not a nerve tumour — but a mechanical overloading problem that produces a very recognisable cluster of symptoms and, critically, has a very identifiable and correctable cause in the majority of cases.
What matters clinically — and what determines the right treatment — is which metatarsal head is overloaded, why it is bearing excessive force, and what is producing that loading pattern. This is information that cannot be determined by pressing on the foot and guessing. It requires pressure mapping.
The 5 Metatarsalgia Symptoms to Know
1. The Pebble-in-the-Shoe Sensation
This is the single most distinctive metatarsalgia symptom and the one that brings most patients to Foot Impact for the first time. The feeling that something small and hard is trapped under the ball of the foot — present with every step, but finding nothing when the shoe comes off.
This sensation is caused by swelling and thickening of the soft tissue and bursa surrounding the inflamed metatarsal heads. The tissue buildup creates a localised fullness underfoot that the brain interprets as a foreign object. It is not imagined and it is not minor — it is a clear signal that the tissue beneath a specific metatarsal head has been under chronic stress.
2. Burning, Aching, or Sharp Pain Under the Toes
The pain of metatarsalgia is typically located in the forefoot — specifically in the area just behind the second, third, and fourth toes, where the middle metatarsal heads are clustered. It ranges from a dull, persistent ache that builds through the day to a sharp, shooting pain with specific movements like walking quickly, climbing stairs, or pushing off during exercise.
A key distinguishing feature: metatarsalgia pain is mechanical. It is consistently worse with weight-bearing and activity, and consistently better with rest. If your forefoot pain is just as bad at rest as during activity, a different diagnosis should be explored.
3. Pain That Builds Through the Day
Unlike plantar fasciitis — which is characteristically worst with the first steps of the morning and eases after walking — metatarsalgia pain typically starts mild and accumulates with activity. Many patients describe feeling fine at the start of a working day, noticing mild discomfort by midday, and experiencing significant pain by late afternoon.
This progressive pattern reflects the cumulative loading of the metatarsal heads over hours of standing and walking. Each step adds a small increment of mechanical stress to already inflamed tissue. By the end of a long day on hard floors, the tissue has been loaded thousands of times and is responding with proportionate pain.
This pattern is particularly relevant for Mumbai's working population — teachers, retail workers, hospital staff, factory workers, and hospitality professionals who routinely spend 6–9 hours on hard floors with inadequate footwear support.
4. Numbness and Tingling in the Toes
When metatarsal heads are chronically inflamed and swollen, they compress the small digital nerves running between them to the toes. This nerve compression produces tingling, numbness, or a pins-and-needles sensation — most commonly in the second and third toes.
This symptom is significant for two reasons. First, it tells you the inflammation has progressed beyond the bone and soft tissue into the nerve territory. Second, if left unaddressed, chronic nerve compression between the metatarsal heads can develop into Morton's neuroma — a more advanced and more painful condition involving a thickening of the nerve sheath that is substantially harder to treat than metatarsalgia at its earlier stages.
5. Callus Formation Under the Ball of the Foot
Look at the sole of your foot. Hard, yellowed skin — callus — forming under the ball of the foot, particularly under one or two specific metatarsal heads, is one of the most useful diagnostic indicators of metatarsalgia. It is your body's protective response to chronic pressure and friction, and it forms precisely where mechanical stress is concentrated.
A callus under the second metatarsal head tells you the second metatarsal is bearing excessive load. Under the third and fourth, the middle forefoot is overloaded. These callus patterns are readable — they are essentially a map of your foot's abnormal loading distribution, and at Foot Impact they inform both diagnosis and orthotic prescription.
Metatarsalgia vs. Similar Conditions — Know the Difference
Forefoot pain is one of the most commonly misdiagnosed areas in podiatry because several conditions produce overlapping symptoms. Here is a clear comparison:
| Condition | Where It Hurts | Key Feature | Key Difference |
|---|---|---|---|
| Metatarsalgia | Ball of foot, behind 2nd–4th toes | Builds through day, pebble sensation | Multiple metatarsal heads involved |
| Morton's Neuroma | Between 3rd and 4th toes specifically | Electric, shooting pain, worse in tight shoes | Single nerve location, often relieved by removing shoe |
| Plantar Fasciitis | Heel and arch | Worst with first morning steps | Pain at heel, not forefoot |
| Sesamoiditis | Directly under the big toe joint | Dull ache, worse pushing off | Pain only under first metatarsal |
| Stress Fracture | Localised to one metatarsal shaft | Sharp pain, swelling, bruising | Worsens rapidly, tender to point pressure |
| Fat Pad Atrophy | General ball of foot | Feels like walking on bones | Common in older adults, cushioning lost |
If you are unsure which of these fits your symptoms, professional assessment is essential. The treatments for these conditions differ significantly — applying metatarsal pads for a stress fracture, for example, delays a diagnosis that requires rest and possibly imaging. Misdiagnosis prolongs suffering unnecessarily.
What Causes Metatarsalgia — The Root Mechanics
Foot Structure: High Arches and Morton's Toe
Two structural factors are the most significant biomechanical drivers of metatarsalgia.
A high-arched foot (cavus foot) does not flatten sufficiently during the midstance phase of walking to distribute load across the whole forefoot. Instead, it transfers the majority of the push-off force onto the central metatarsal heads — the second, third, and fourth — which were not designed to bear this concentrated load repeatedly. High arches also produce a stiffer foot with less shock absorption, meaning impact forces are transmitted more directly to the metatarsal heads rather than being absorbed through normal arch deformation.
Morton's toe — where the second toe is longer than the big toe — shifts excessive load onto the second metatarsal head, which is forced to function as the primary push-off point on a foot that anatomically should be pushing off through the first metatarsal. Over thousands of steps per day, this structural mismatch produces predictable metatarsal head overloading and pain.
Footwear — Particularly High Heels and Narrow Toe Boxes
High heels mechanically shift the body's centre of gravity forward, concentrating the majority of standing and walking load on the forefoot. The higher the heel, the greater the percentage of body weight borne by the metatarsal heads rather than the heel. Regular high heel use in people with any forefoot structural predisposition dramatically accelerates metatarsalgia development.
Narrow toe boxes compress the metatarsal heads together, reducing the natural spread of the forefoot that helps distribute load. Pointed-toe shoes effectively eliminate the structural width advantage the foot naturally has during weight-bearing.
For Mumbai's professional working population — where formal and fashion footwear is worn for 8–10 hours daily — this is a major and underappreciated driver of forefoot pain.
Weak Forefoot and Intrinsic Foot Muscles
The small intrinsic muscles of the foot — the lumbricals, interossei, and flexor digitorum brevis — play a critical role in stabilising the metatarsophalangeal joints during walking and protecting the metatarsal heads from excessive direct loading. When these muscles are weak or fatigued, the metatarsal heads lose their dynamic support and bear greater impact force with every step.
This weakness is extremely common in people who wear supportive footwear most of the time, as the intrinsic muscles are chronically underloaded and gradually decondition. It is also common after periods of reduced activity or following any lower limb injury that has altered gait patterns.
Sudden Increase in Activity
One of the most common presentations at Foot Impact is metatarsalgia that developed after a significant increase in activity — starting a running programme, returning to sport after a long break, or a job change involving substantially more standing. The metatarsal bones and soft tissues adapt to load over time, but when activity increases faster than the adaptation process, the forefoot structures are exposed to forces they are not yet prepared to absorb.
Excess Body Weight
Because the metatarsal heads bear a direct proportion of body weight with every step, any increase in weight increases the load on the forefoot proportionally. Even modest weight gain can tip a marginally compensated forefoot into symptomatic metatarsalgia in someone with an underlying structural predisposition.
How Metatarsalgia Is Diagnosed at Foot Impact — Beyond Guessing
The most important thing that separates effective from ineffective metatarsalgia treatment is diagnostic accuracy at the start. Knowing that the ball of the foot hurts is the symptom. Knowing which metatarsal head is overloaded, why it is overloaded, and what is driving that pattern during actual walking — that is the diagnosis.
At Foot Impact's clinics in Andheri West and Khar West, Mumbai, every metatarsalgia assessment includes:
Clinical History Duration, onset pattern, which activities make it worse and better, occupational demands, footwear habits, and any relevant history including previous foot injuries, diabetes, or inflammatory conditions.
Physical Examination Metatarsal head palpation to identify which specific heads are tender, plantar callus pattern assessment, toe alignment and metatarsophalangeal joint mobility testing, and basic neurological screening to assess digital nerve function and rule out early Morton's neuroma.
Computerised Pedobarography — Pressure Mapping This is the diagnostic step that changes the treatment outcome. A pedobarographic scan maps the pressure distribution across the entire plantar surface of your foot during both standing (static) and walking (dynamic). It identifies exactly which metatarsal heads are bearing excessive load, the magnitude of that overloading, and whether it is occurring throughout stance or specifically during the push-off phase.
The dynamic scan is particularly important — forefoot loading patterns during walking are substantially different from those captured in a static scan, and most metatarsalgia drivers only become apparent during the dynamic movement cycle. This is why generic insoles — designed without this data — so frequently fail to provide lasting relief. They add cushion to the entire forefoot rather than offloading the specific overloaded structures.
Foot Structure and Gait Assessment Arch type, metatarsal formula (relative length of metatarsals), hindfoot alignment, and overall lower limb biomechanics are assessed as an integrated system — because forefoot overloading rarely occurs in isolation from the broader mechanics of how the foot and leg move together.
Footwear Review Every pair of shoes the patient regularly wears is assessed. Worn heel and forefoot patterns in footwear are among the most revealing diagnostic indicators available, often confirming loading patterns before the pressure scan is even run.
Metatarsalgia Treatment — What Actually Works
Custom Orthotics with Metatarsal Padding
For the majority of metatarsalgia cases, a correctly prescribed custom orthotic is the most effective single intervention available. The key word is correctly prescribed — the orthotic must be designed from the pressure mapping data to offload the specific overloaded metatarsal heads, not simply provide general forefoot cushioning.
At Foot Impact, custom orthotics for metatarsalgia incorporate a metatarsal dome or bar — a precisely positioned elevation behind the overloaded metatarsal heads. This lifts and separates the metatarsal heads slightly, redistributing load from the central heads toward the first and fifth metatarsals where it can be better tolerated. The position and height of this element is determined by the pressure mapping data — placed incorrectly, it transfers load to the wrong structure and worsens the problem.
Patients with metatarsalgia who receive correctly positioned custom orthotics from pressure mapping data consistently report meaningful pain reduction within 3–4 weeks.
Footwear Modification — Specific, Not Generic
The right footwear recommendation for metatarsalgia depends on the cause. For high-arch-driven cases, a shoe with a rocker sole — which reduces the force required at push-off and therefore the peak load on the metatarsal heads — is the specific recommendation. For cases driven by forefoot compression from narrow toe boxes, a shoe with adequate forefoot width is the priority. For cases involving Morton's toe, a specific heel-to-toe drop and metatarsal position within the shoe matters.
Generic advice to "wear wider shoes" is a starting point, not a prescription. At Foot Impact, footwear guidance is specific to your foot type, loading pattern, and the practical realities of your daily life in Mumbai.
Intrinsic Foot Muscle Strengthening
A targeted exercise programme to strengthen the intrinsic foot muscles reduces the dynamic load on the metatarsal heads by restoring the active support that these muscles are supposed to provide. Exercises including toe spread and lift progressions, towel scrunches, short foot exercises, and single-leg balance work under progressive loading are prescribed based on the patient's current strength baseline and rate of progression.
These exercises are most effective as a complement to orthotics and footwear correction — they address the muscular component of forefoot overloading while the orthotics address the structural component.
Activity Modification During Recovery
During the acute phase — particularly for cases involving significant inflammation or early stress response in the metatarsal bone — activity modification is important. High-impact activities (running, jumping, prolonged walking on hard surfaces) should be reduced or temporarily avoided to allow inflamed tissue to settle. This does not mean complete rest — low-impact activity that maintains fitness without loading the forefoot is appropriate and preferable.
The key is graduated return to full activity rather than abrupt resumption once pain eases — the pattern that most commonly produces relapse.
Footwear Rotation and Workplace Adjustments
For Mumbai's working population — teachers, healthcare workers, retail staff, factory and hospitality workers — the workplace environment is a major metatarsalgia driver that standard treatment advice rarely addresses. Anti-fatigue matting at standing workstations, footwear rotation to alter repetitive loading patterns, and specific footwear choices for different work environments are practical interventions that can produce dramatic reductions in daily forefoot pain without any other change.
If prolonged standing is part of your working life, ask about our occupational foot assessment at Foot Impact. It is one of the most practically impactful assessments we offer.
When Metatarsalgia Becomes Something More Serious
Morton's Neuroma
Untreated metatarsalgia that persists for months and involves ongoing nerve compression between the metatarsal heads can progress to Morton's neuroma — a thickening of the nerve sheath between the third and fourth metatarsals that produces sharp, electric, shooting pain and more persistent numbness in the affected toes. Morton's neuroma is harder to treat than metatarsalgia at an earlier stage and may require corticosteroid injection or, in advanced cases, surgical intervention.
If your forefoot pain includes shooting or electric sensations between specific toes, a Morton's neuroma assessment should be included in your diagnosis.
Metatarsal Stress Fracture
Chronic repetitive overloading of a metatarsal head can progress from soft tissue inflammation to a stress response in the bone itself — and in more severe cases, to a metatarsal stress fracture. A stress fracture produces more localised, more severe pain with point tenderness over a specific metatarsal shaft, may be accompanied by swelling and bruising, and typically worsens rapidly with continued loading.
If your ball-of-foot pain has suddenly become significantly worse, is associated with visible swelling, or makes walking difficult, imaging should be obtained to rule out a stress fracture before continuing activity.
Preventing Metatarsalgia From Returning
Once metatarsalgia has been properly treated, the priority is preventing recurrence. The following measures are consistently effective:
- Wear custom orthotics prescribed from your pressure mapping data consistently — not just when pain is active. The mechanics that were overloading your metatarsal heads are still present when you are pain-free.
- Replace athletic footwear every 500–600 km — worn forefoot cushioning increases metatarsal head impact substantially
- Avoid prolonged barefoot walking on hard floors, particularly tiles and marble which are the most common flooring in Mumbai homes and workplaces
- If you are a runner, increase mileage by no more than 10% per week — the most common cause of runner's metatarsalgia is too much, too fast
- Perform intrinsic foot strengthening exercises consistently as part of your regular routine, not just during a pain episode
- Rotate footwear to alter repetitive stress patterns across the forefoot
For diabetic patients specifically — metatarsalgia is a condition that requires particularly close monitoring, because the reduced sensation associated with diabetic neuropathy means the pain warning system is unreliable. Pressure sores and ulcers over overloaded metatarsal heads can develop and progress seriously in diabetic patients without the level of pain that would prompt attention in a non-diabetic person. Regular podiatric review and pressure mapping are essential components of diabetic foot care.
👉 Book Your Metatarsalgia Assessment at Foot Impact, Andheri West, Mumbai →
Frequently Asked Questions About Metatarsalgia
Q1. Can metatarsalgia heal on its own without treatment? Mild, early-onset metatarsalgia triggered by a temporary change in activity — a long walking holiday, new footwear, a sudden increase in training — may settle with rest and footwear change. However, metatarsalgia driven by an underlying structural factor like high arches, Morton's toe, or weak forefoot muscles will reliably return once activity resumes. The underlying mechanical cause continues to apply the same stress to the same structures with every step, regardless of how long pain-free periods last. Without correcting that cause, the condition is being managed temporarily rather than resolved properly.
Q2. Why is my metatarsalgia not getting better with the insoles I bought from the pharmacy? Pharmacy insoles provide generalised forefoot cushioning. They reduce impact across the entire forefoot, which may temporarily relieve discomfort. What they cannot do is selectively offload a specific overloaded metatarsal head — because they are not designed from the pressure mapping data that shows which head is overloaded and by how much. A correctly positioned metatarsal dome at the right height, in the right location relative to your specific loading pattern, is a fundamentally different intervention. It is the difference between turning down the volume across all speakers equally and reducing the specific speaker that is too loud.
Q3. How do I know if I have metatarsalgia or Morton's neuroma? The distinction matters for treatment. Metatarsalgia typically produces diffuse burning and aching across the ball of the foot, is worse with prolonged activity, and improves with rest. Morton's neuroma produces a more localised electric or shooting pain, often described as a shock between the third and fourth toes specifically, and is frequently triggered by the compression of a narrow shoe and relieved — at least temporarily — by removing the shoe and rubbing the forefoot. However, the two conditions commonly co-exist, and distinguishing them accurately requires clinical examination and in some cases ultrasound imaging. A podiatric assessment at Foot Impact will identify which condition is driving your symptoms and whether both are present.
Q4. Is walking barefoot helpful or harmful for metatarsalgia? Harmful in most cases, particularly in urban Indian environments. Walking barefoot on hard floors — marble, tile, concrete, the surfaces that dominate Mumbai homes and workplaces — exposes the metatarsal heads to direct, unabsorbed impact with nothing between them and a rigid surface. For people with high arches or depleted forefoot fat pads, this is significantly more damaging than walking in supportive footwear. Supportive indoor footwear or recovery sandals with forefoot cushioning are strongly recommended during any active metatarsalgia episode, and maintained thereafter as a preventive measure.
Q5. Can metatarsalgia cause pain in my knees or lower back? Yes — and this is more common than most people realise. When forefoot pain alters your walking pattern, the compensations travel upward through the kinetic chain. Subconsciously offloading a painful forefoot typically means shifting weight to the heel, the outer foot, or the opposite leg — patterns that create abnormal loading at the ankle, knee, and hip. Patients presenting to Foot Impact with unexplained knee or lower back pain are often found on pressure mapping to have significant forefoot loading asymmetry as a contributing driver.
Q6. How long does recovery from metatarsalgia typically take? For early-stage metatarsalgia addressed with correctly prescribed orthotics and footwear modification, most patients notice meaningful improvement within 3–4 weeks and reach full symptomatic resolution within 8–10 weeks. For chronic cases that have been present for 6 months or more — particularly those involving secondary nerve compression or early stress responses in the metatarsal bone — recovery typically takes 3–4 months of consistent treatment. The variable that most reliably determines recovery speed is how early treatment is started. A patient who comes to Foot Impact within the first 4–6 weeks of metatarsalgia symptoms recovers substantially faster than one who has been managing independently for a year.
Conclusion — The Pebble Under Your Foot Has an Explanation
That burning, aching, pebble-in-the-shoe feeling under the ball of your foot is not something to walk off, ignore, or temporarily relieve with a cushioned insole and hope for the best. It is a mechanical signal from a specific overloaded structure — and that structure can be identified precisely, offloaded correctly, and returned to pain-free function in the majority of cases.
At Foot Impact, we see metatarsalgia patients every week in Mumbai who have been managing this pain for months or years with pharmacy products that were never going to resolve it, because they were never designed around the actual cause. A 45-minute assessment with pressure mapping changes the entire treatment picture — it replaces guesswork with data and generic advice with a plan specific to your foot, your loading pattern, and your daily life in Mumbai.
If the ball of your foot has been telling you something, it is time to find out exactly what.
Book your metatarsalgia assessment at Foot Impact, Andheri West, Mumbai →