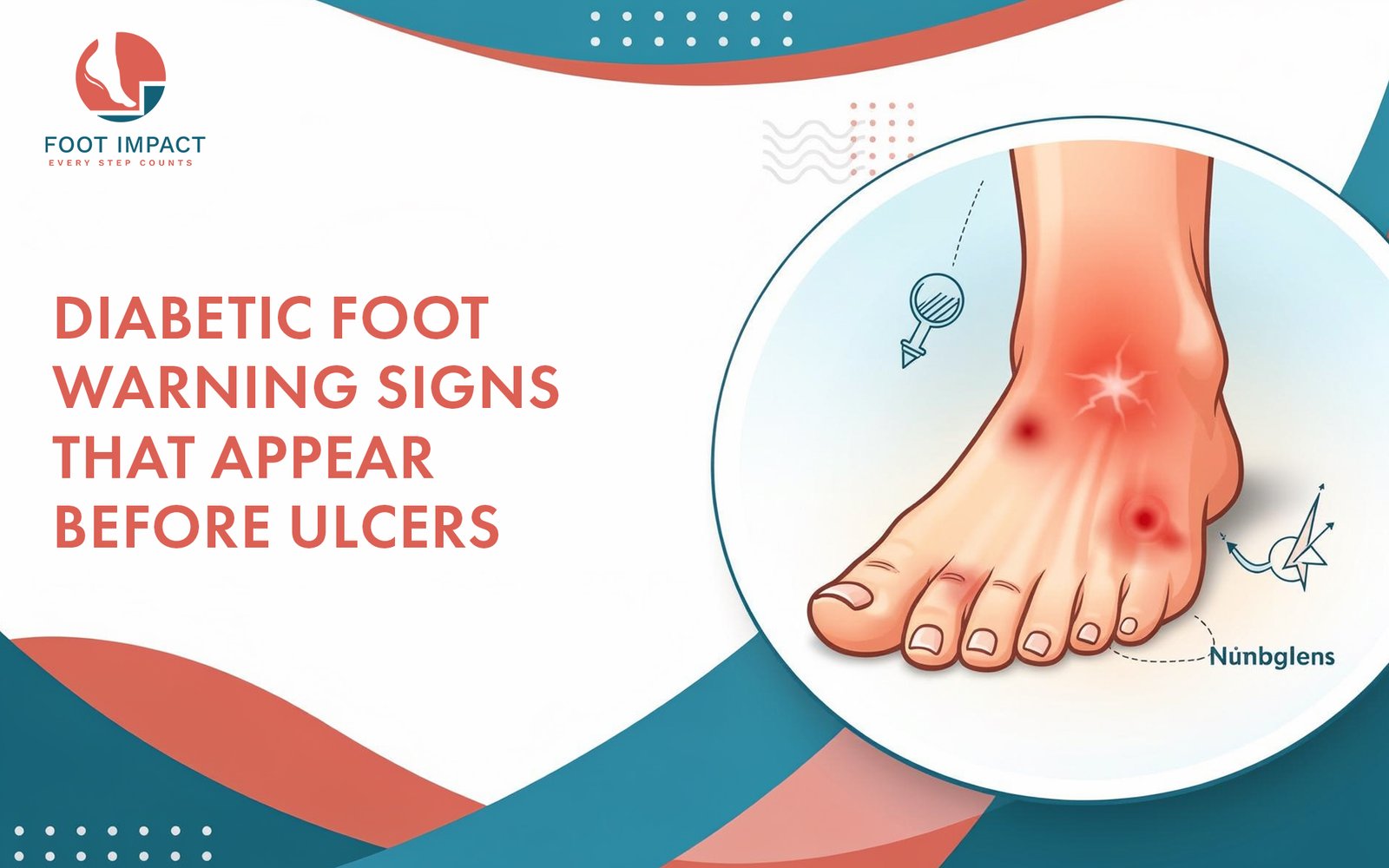
Diabetic Foot Warning Signs That Appear Before Ulcers
Diabetic foot warning signs rarely begin with dramatic symptoms. In most cases, they appear quietly — a patch of dry skin, mild numbness, a small color change, or a callus that feels slightly different than usual. Because these early changes are subtle, many people living with diabetes overlook them. Unfortunately, ignoring these early diabetic foot warning signs can allow minor problems to progress into infections or ulcers.
Foot ulcers are one of the most serious complications of diabetes. However, they almost never appear suddenly. They are usually the result of untreated nerve damage, poor circulation, pressure points, or unnoticed skin breakdown. Recognizing diabetic foot warning signs early can dramatically reduce the risk of severe infection, hospitalization, or even amputation.
This guide explains the earliest symptoms to watch for, why they occur, and how podiatrists help prevent complications before they become dangerous.
Why Diabetic Foot Warning Signs Appear
Diabetes affects the body in several ways. Two major complications increase the risk of foot problems:
Peripheral neuropathy (nerve damage)
Peripheral artery disease (reduced blood flow)
According to the Centers for Disease Control and Prevention, high blood sugar over time can damage nerves and reduce circulation, especially in the feet. When sensation decreases, small injuries may go unnoticed. At the same time, reduced blood flow slows healing.
The World Health Organization also highlights that diabetic foot complications are a leading cause of preventable hospital admissions worldwide.
In simple terms: when feeling decreases and healing slows, minor skin changes can escalate quickly.
Early Diabetic Foot Warning Signs to Watch For
1. Numbness, Tingling, or Burning Sensation
One of the earliest diabetic foot warning signs is a change in sensation. You may feel:
Pins and needles
Mild burning
Reduced ability to feel temperature
A “cotton-like” feeling under the feet
These symptoms suggest peripheral neuropathy. Without proper sensation, you may not notice blisters, cuts, or pressure injuries.
2. Persistent Dry or Cracked Skin
Dry skin may seem harmless, but for people with diabetes, it can be an early red flag. Autonomic neuropathy reduces sweat production, causing excessive dryness. Cracks (especially on the heels) can become entry points for bacteria.
If untreated, these cracks may deepen and evolve into open wounds.
3. Calluses That Grow Quickly
Calluses form where pressure is excessive. In diabetes, thick calluses may hide bleeding underneath. Over time, this pressure can break down skin layers and lead to ulcers.
If you notice calluses forming repeatedly in the same spot, it may signal abnormal pressure distribution.
Learn more about professional diabetic foot care and pressure assessment services to prevent complications.
4. Color Changes in the Skin
Subtle color changes are important diabetic foot warning signs. Watch for:
Redness in one area
Bluish or pale skin
Darkened patches
Localized warmth
Redness may indicate inflammation or early infection. Pale or bluish tones can signal poor circulation.
The American Diabetes Association advises individuals with diabetes to monitor daily for skin color changes, as they often precede ulcer formation.
5. Swelling in One Foot
Swelling without injury should never be ignored. It may indicate infection, poor circulation, or Charcot foot — a serious complication involving bone weakening.
Early diagnosis dramatically improves outcomes.
6. Toenail Changes or Fungal Infections
Thickened, yellow, or brittle nails can harbor fungal infections. If untreated, nail problems may injure surrounding skin and create open wounds.
Explore our ingrown and fungal toenail treatment services to reduce infection risk.
Why Small Foot Problems Escalate Quickly in Diabetes
The progression often follows this pattern:
Minor pressure → Callus formation → Skin breakdown → Bacterial entry → Ulcer → Infection
According to the National Institute of Diabetes and Digestive and Kidney Diseases, early detection and preventive care significantly reduce amputation risk.
When diabetic foot warning signs are ignored, healing delays allow bacteria to multiply. Therefore, proactive monitoring is essential.
High-Risk Individuals Who Should Be Extra Vigilant
You are at higher risk if you:
Have had diabetes for more than 10 years
Have uncontrolled blood sugar levels
Smoke
Have previous foot ulcers
Experience reduced sensation
Annual foot examinations are strongly recommended for all diabetic patients.
How Podiatrists Prevent Diabetic Foot Ulcers
Professional diabetic foot management includes:
Sensory testing
Circulation assessment
Pressure mapping
Callus management
Nail care
Footwear guidance
At FootImpact, we offer comprehensive diabetic foot assessment and preventive care services to detect diabetic foot warning signs before ulcers develop.
Timely intervention often prevents hospitalization.
Daily Foot Care Routine for Prevention
Adopting a simple routine can dramatically reduce risk:
Inspect your feet daily (use a mirror if needed).
Wash gently and dry thoroughly, especially between toes.
Apply moisturizer (avoid between toes).
Trim nails carefully.
Wear well-fitted, supportive footwear.
Never walk barefoot.
Consistency is critical.
Comparison: Early Action vs Delayed Treatment
Recognizing diabetic foot warning signs early changes the entire trajectory of care.
When to Seek Immediate Medical Attention
Seek urgent care if you notice:
Open wounds
Pus or discharge
Fever with foot pain
Rapid swelling
Blackened tissue
Prompt treatment can prevent serious complications.
Frequently Asked Questions (FAQ)
1. What are the earliest diabetic foot warning signs?
The earliest signs include numbness, dry cracked skin, calluses, color changes, and mild swelling.
2. How often should diabetics check their feet?
Daily self-checks are recommended, along with professional evaluation at least once per year.
3. Can foot ulcers be prevented completely?
While not all ulcers are preventable, early identification of diabetic foot warning signs significantly reduces risk.
4. Are minor cuts dangerous for diabetics?
Yes. Even small cuts can become serious due to delayed healing and infection risk.
5. What footwear is best for diabetic patients?
Supportive, well-cushioned shoes that reduce pressure points are ideal.
Conclusion
Diabetic foot warning signs do not appear dramatically. They often begin quietly — a numb toe, dry heel, small callus, or mild discoloration. Yet these subtle symptoms can precede serious complications if ignored.
The key to preventing ulcers is vigilance. Daily self-checks, proper footwear, blood sugar control, and regular podiatric evaluations significantly reduce risk. By identifying diabetic foot warning signs early, you protect not just your feet but your overall mobility and quality of life.
If you live with diabetes, proactive foot care is not optional — it is essential. Early intervention saves limbs, preserves independence, and prevents life-altering complications.